 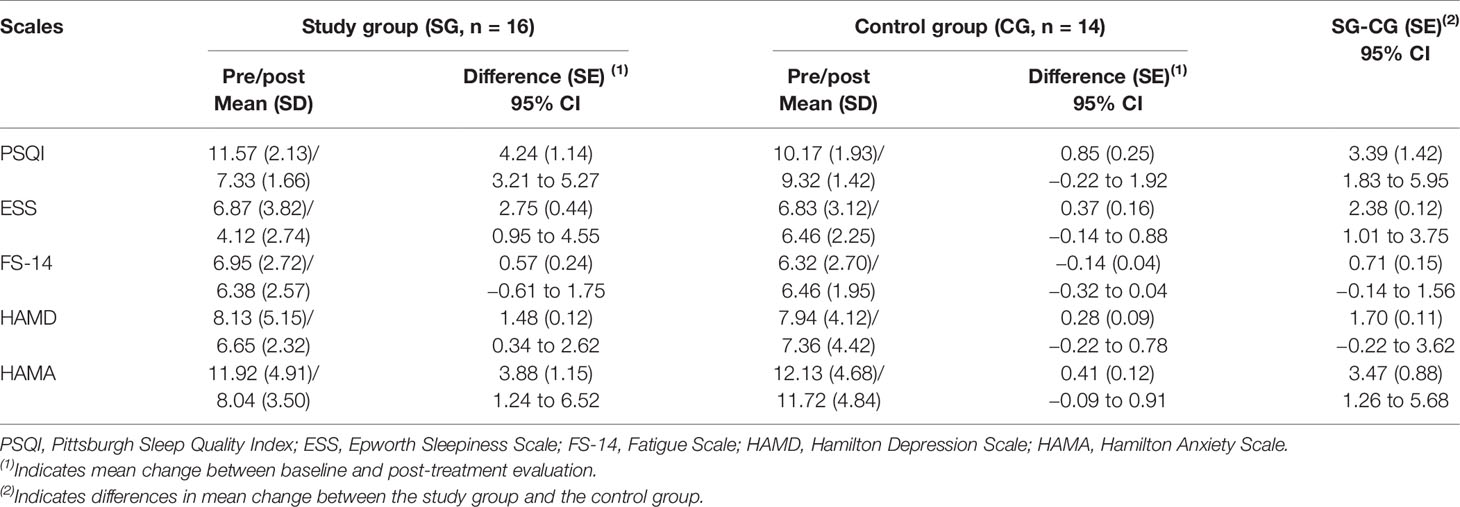
A customized bed alarm that plays a soothing message from a familiar person, triggered by patient movement, has shown preliminary benefit in a small series of RBD patients with treatment-refractory disease. Nonpharmacologic therapy revolves around safety measures, for example use of a hospital bed with padded bed rails or removing potentially dangerous objects from near the bed. Because RBD frequently manifests in patients who will ultimately develop a synucleinopathy, and because most treatment studies of RBD have included a mix of patients with and without diagnosed PD, this section will consider RBD treatments used in patients with and without comorbid PD. Treatment for RBD is generally recommended when there is substantial risk of injury to the patient or bed partner, or when there is severe sleep disruption. Considered to be a disorder of both nocturnal movement and dream content, RBD is associated with a lack of atonia in REM sleep, and patients act out vivid and frequently violent dreams. RBD is a parasomnia that occurs in 15–59 % of PD patients, more commonly in those who are older, male, have sudden sleep attacks, experience orthostatic hypotension, and have PD not associated with prominent tremor. Significant improvement in PD Sleep Scale-2 scores (co-primary outcome) No improvement in primary measure of sleepiness (ESS) Improvement in ESS scores improvement on one (not all) subjective fatigue ratings No improvement in ESS scores, Multiple Sleep Latency Test, or subjective fatigue ratings No improvement in ESS scores improvement in motor fatigue but not subjective fatigue ratings Improvement in ESS scores no improvement in Maintenance of Wakefulness Test Improvement in Epworth Sleepiness Score (ESS) scores Improvement in subjective primary outcome no improvement in objective primary outcomeĮxcessive daytime sleepiness and/or fatigue Improvements in Insomnia Severity Index and Scales for Outcomes in Parkinson’s Disease-night (co-primary outcomes) Total sleep time (by diary) not improved several secondary measures of insomnia did improve Motor function and quality of life worsened. Improvements in some, but not all, subjective measures of insomnia. Group cognitive–behavioral therapy for insomnia, 6 sessions of 90 mins, combined with light therapy Improvement in Clinical Global Impression (CGI)-change scoresĭecrease in bedpartner-reported RBD episodes 
Melatonin, 3 mg (most subjects did not have PD) Rapid eye movement behavior disorder (RBD) 
In those patients with early morning motor dysfunction and disrupted sleep, the rotigotine patch provides significant benefit. Optimal treatment of restless legs syndrome and obstructive sleep apnea in PD are not yet established, although a trial of continuous positive airway pressure for sleep apnea was recently completed in PD patients. Use of the wake-promoting agent modafinil results in significant improvement in subjective measures of excessive daytime sleepiness, but not of fatigue. Optimal treatments for insomnia in PD have yet to be determined, but preliminary evidence suggests that cognitive–behavioral therapy, light therapy, eszopiclone, donepezil, and melatonin might be beneficial. For rapid eye movement sleep behavior disorder, melatonin and clonazepam are most commonly used, while rivastigmine might be a useful option in patients whose behaviors are refractory to the former. Sleep disorders are common in patients with Parkinson’s disease (PD), and preliminary work has suggested viable treatment options for many of these disorders.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
